In December 2016 I spent a month in the hospital with respiratory problems and getting a trach. The first half of the story was chronicled in a series titled “Pray That They Listen to the Man with No Voice” about my time in St. Vincent ICU. The second part title “Holiday Hospital” is about the rest of December including Christmas in St. Vincent Seton Specialty Hospital. I recently was going to share the story with a friend and realized that I had not yet completed the Holiday Hospital series. It’s been over three years since the events happened but I never did complete the story. So I will try once again to finish it up. This is part 10 in the “Holiday Hospital” series. Here is an index to all of the entries in this series.
Prison Break
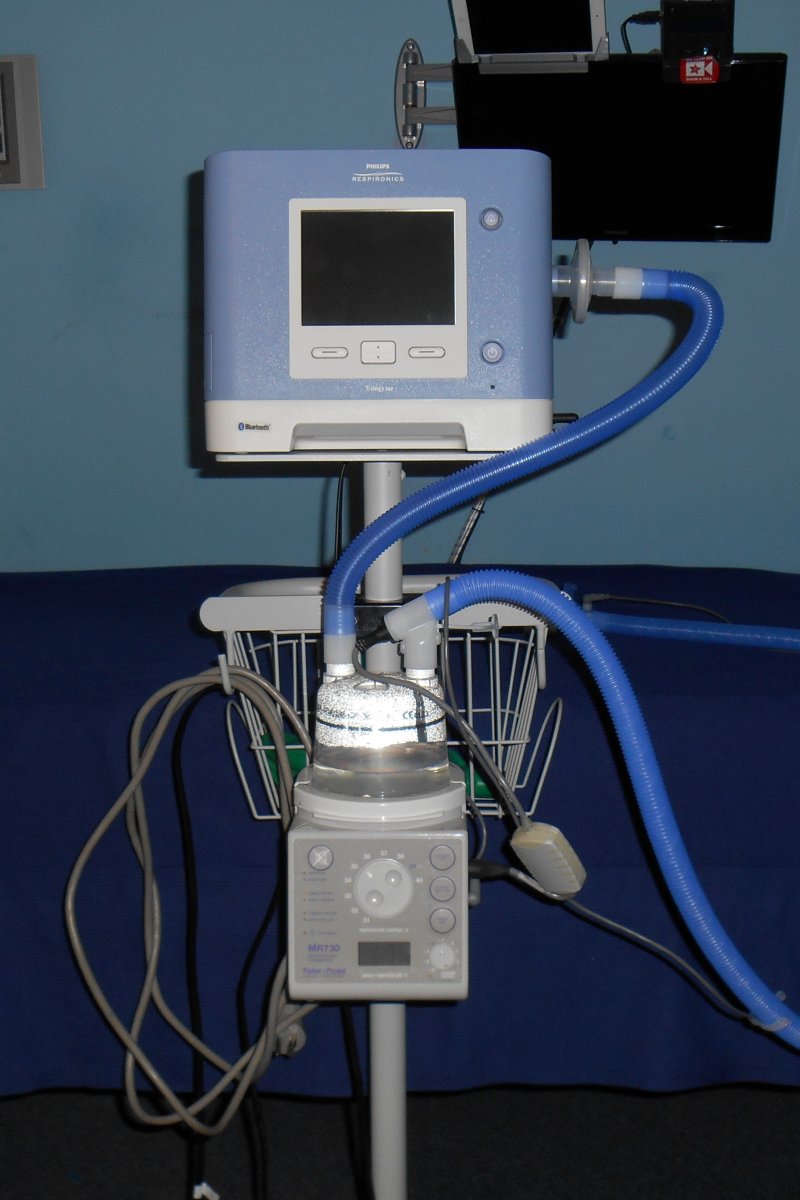
In the previous installment of this story I told about the test that my dad had to pass by spending the night in the hospital with me and proving that he could handle my ventilator and trach issues. It had been a really rough night and neither of us had gotten much sleep but we had passed the test despite some minor mistakes. Theoretically all that had to happen was for the doctors or nurse practitioners to sign some forms and we would be on our way home. The respiratory therapist was planning on meeting us at my house to bring a bunch of supplies. We already had the new ventilator and will be taking it home with us.
Checking out of a hospital always takes longer than you think it should. You are anxious to get home and bureaucracy always moves at a snail’s pace. Over the years I’ve learned you just have to be patient and let the system go on its own pace. Here is a Facebook post I made at 6:50 a.m. Just as a reminder anytime you see this little Facebook icon is a link to a Facebook post related to when I’m talking about. [12/28/2016 6:50 AM] 
Dad got me up and dressed and we began packing up a bunch of my stuff and hauling it out to the van. Unfortunately we hit a major snag. In theory my trach should be replaced once a month. For the first replacement it should be done by a doctor who would train my dad how to do subsequent replacements. We are describing events of December 28 and I had had the trach since December 7 so the soonest I would’ve really needed a replacement would’ve been January 7. But for some reason the powers that be decided they would not let me out of the hospital until I had a definitive appointment to change the trach.
I tried to convince them that it was not an immediate need. If they were so concerned about getting the trach changed why didn’t they just go ahead and change it right now if that was a prerequisite for me getting out. They didn’t really have anyone who was willing to do that. As I mentioned in previous installments there was really only one doctor covering the entire facility. Everything else was run by nurse practitioners and therapists and the doctor wasn’t available at the time.
They were trying to get in touch with my regular ENT doctor but he was on vacation over the holidays. The receptionist who booked his appointments didn’t know if he would even do that kind of thing in the office. Here is a Facebook video that I shot at 11:43 AM that shows me up and dressed and ready to go and basically telling the same story I just told in the past couple of paragraphs. In the video I said that I had had the trach installed on December 9 but it was actually December 7.
I impatiently roamed the halls almost all afternoon occasionally arguing with the case manager Michelle trying to get her to sign off on releasing me without getting the trach change nailed down. I even bribed her with a little 3D printed Christmas tree ornament which she really liked but it didn’t move things along any faster. [12/28/2016 2:02 PM] 
Happy Holidays
While I was killing time waiting on my release from prison I managed to strike up conversations with some of the other staff. There were respiratory therapists and nurses just standing around the hallway in between doing whatever needed to be done. So I had some nice conversations with them. One of the people who I had seen every day was a woman who would sweep the rooms and emptied the wastebaskets. She was obviously a Muslim because she always wore a hijab headdress. I often wondered what it was like for her to work in a place where there were perhaps no other Muslims and everyone was going around wishing one another Merry Christmas. On several occasions, especially this one, I thought about saying to her “as-salamu alaykum” which is a tradition Islamic greeting that translates to “peace be upon you”. But I really didn’t know how it would be received and I don’t know any other Arabic phrases or words and I didn’t want to have her think I could actually speak Arabic.
A few months later I would have a respite nurse named Mohammed Tahir who became a good friend. We frequently had long discussions about religion. He was very curious about other faiths and had studied them on his own. I would answer his questions about Catholic Christianity and he would answer my questions about Islam. If I had had my experience with him I would’ve been much more open to reaching this woman with the Arabic greeting.
It Fell off a Truck
Among the things that they do for you as you are leaving the hospital is make sure that you have all of your necessary prescriptions. Just about everything that I was taking except for the new prostate medicine was stuff that I was already taking before going into the hospital. And if I missed a day or two of the prostate drug it wasn’t going to be any big deal. The one thing I was worried about was albuterol. It is a liquid that you put into your nebulizer to help clear your lungs. It comes a little plastic ampoules where you twist off the top and pour it into the nebulizer. I was concerned that I might need a breathing treatment before dad could get to the pharmacy and get that prescription filled. So we talked to one of the respiratory therapists and she was able to slip us a couple of ampoules of the medicine to take home with us. We said to her “I wonder where this came from? We just found it lying here.” She said “Maybe it fell off a truck and you found it.” We had a big laugh. Little did we know that filling that prescription was going to be more difficult than we anticipated so it was a good thing she got us a few free samples.
Free at Last
I don’t know what time we finally got out of the hospital but my notes say that we didn’t get home until 5 PM. We still had to meet the respiratory therapist at my house so that he could deliver the supplies. They arranged to get me a tentative appointment with my ENT doctor sometime in early January to change the trach. Unfortunately it was something like 8 AM which there was no way I was going to be there that early. A few days later I called to reschedule it at a more convenient time and we didn’t actually change it until January 12. And guess what… the world did not come to an end and I did not die because my trach was changed a few days later than scheduled. But I had wasted the entire day until they made arrangements for no good reason whatsoever.
As we were going out the door escorted by the case manager Michelle, she acted as though she had achieved some sort of victory. She had told us that it would take 2 weeks to get the ventilator arranged and I was being released from the hospital almost exactly 2 weeks after I entered. I explained to her that first of all there was no reason on earth the process should’ve taken that long. Also we had been trying to arrange the ventilator for five or six days back when I was still at St. Vincent before ever got to her facility. And that time had been completely wasted. Essentially we had to start from scratch when we moved to the new hospital. Furthermore there was absolutely no medical reason why I had to be in the hospital that long except for the bureaucracy of obtaining the ventilator and there was no reason that she needed to keep me in the hospital all that afternoon. So I didn’t acknowledge anything she did as a victory and I told her so in as nice yet firm as I could muster under the circumstances.
A Mountain of Supplies
As mentioned above, we got home about 5 PM. We had called the respiratory therapist Josh to meet us there and he arrived shortly after we did. He brought in boxes upon boxes upon boxes of supplies most of which we didn’t know how to use or even if we would ever need them. By the time he left they were piled high on our dining room table and all over the family room floor. We had no idea where we were going to store the stuff. He came back again the next day with even more supplies and eventually brought the high flow air compressor that I was going to use to humidify my trach when I wasn’t on the ventilator. As I previously reported in the end we never used that compressor very much and ended up getting rid of it after having to fight hard to get it in the first place.
Dad still had to unload my ventilator and all of my clothes, laptop computer etc. out of the van. I did a G-tube feeding and went to bed. We were both incredibly exhausted but especially dad because he had not slept well in the hospital with me the night before on that horrible Guantánamo Bay worthy cot.
The First Day Home
The first night at home was uneventful. Dad and I both got caught up on our sleep. The only problem we have was when we got me off of the ventilator the next morning we did not fully deflate the cuff in my trach and so I had a bit of difficulty breathing when he put in the talking valve. We eventually figured it out and I was able to breathe much easier. We had yet another visit from the respiratory therapist who brought even more supplies. We also had a visit from 2 nurses from St. Vincent were going to come for a half-hour a day a couple times a week to check up on me. I’m not really sure why we had them but in one incident they turned out to be useful.
I was able to get shaved again which felt good. We were not able to get all my prescriptions and as it turned out the nebulizer prescription for albuterol was going to be difficult to fill. Apparently you need some sort of special authorization for Medicare/Medicaid to pay for it. Of course the prescription was signed by either a doctor or nurse practitioner from Seton Hospital. I had no idea who they were. I didn’t recognize the name. We tried to get in touch with them through the case manager Michelle but we could not contact her over the weekend. Finally one of my St. Vincent nurses proved her worth that Saturday by getting on the phone with the pharmacist and reading him the riot act. She gave a real tearjerker scary argument saying that she didn’t want to be responsible if I went into respiratory arrest because I didn’t have my nebulizer medication. He finally relented and filled the prescription. As it turned out I did need a few treatments over the next several days but in the long term I rarely needed nebulizer treatments. I think that initial batch of albuterol lasted me over a year and I think we eventually threw some of it out because it expired and we got another prescription for my regular doctor. [12/29/2016 2:05 PM] 
Epilogue
I continued to take notes about my day today progress from the time I got home through January and parts of early February. The story isn’t really interesting in retrospect so I’m not going through all of the detail that I did about the hospital stays. In summary here are some highlights of things I went through.
Typically if I needed to call dad while I was in bed and he was in the living room watching TV or asleep in the recliner, I would just yell really loud. When he was in the bedroom I had a buzzer that I can push and it would ring the alarm in the bedroom. But when I was on the ventilator, I couldn’t call at all by voice. So I had to modify a wireless remote that I had built for the living room to include a buzzer like the one we had in the bedroom.
After spending the entire month in the hospital using a spit cup with a lid and a straw in it, we decided using a regular glass tumbler with no lid and a straw was a bad idea. Dad got some plastic cups that he found in our cabinets that had been left over from some event my mom had hosted years ago. We couldn’t find lids that would fit so I made them out of ninja flex plastic on my 3D printer. I still use plastic cups with 3D printed lids to this day.
I had a follow-up doctor appointment with my family doctor, my pulmonary doctor, and my ENT who trained us how to change the trach. He changed it with my dad watching and then asked dad to remove it and put it back in again while the doctor watched. It all went very smoothly. However a month later when dad tried to change it on its own, we had great difficulty getting the old one out and the new one back in. We got it eventually but it was very difficult and clear the lots of blood. This continued for several months so I made another appointment hoping that he could show us what we were doing wrong.
The doctor sort of looked at us funny and you could tell he was thinking “Didn’t we are ready show you how to do this?” When he went to take out the old trach, he had the same difficulty getting the old one out that we did. When he tried to put in the new one, he could not get it in at all! I was so happy that he was having the same difficulty we did. He finally started probing around my opening using the Yankaur and discovered that my opening was not straight in. It actually slopes downward slightly. So then he tried putting in the trach again but this time angling it downward. It popped right in with little difficulty. Dad and I continued use this method. Since dad passed away in February, my sister Carol has been changing the trach on a monthly basis and it works okay using this downward angle method. I’ve had some trach failures at inappropriate times. The balloon that blows up the internal cuff got damaged and would not inflate. The worst time once the night before my dad’s funeral. I could not put on the ventilator and had to try to sleep without it. I got about three hours sleep and then had to go deliver the eulogy for my dad which you can find here. Other than that we’ve had few problems with the trach these past 3 years.
For the first several weeks I had lots of problems with my back brace not fitting very well. I also had problems with my hips. I just wasn’t used to sitting up in my wheelchair all day every day. Over the course of the next months things began to slowly get back to normal. However some days I had to go back to bed early. While it is possible to do a G-tube feeding in bed, in theory you need to be propped up at an angle for at least 30 minutes after a feeding. Otherwise you risk reflux and aspiration. So we made the decision after all these many years to finally get a hospital bed. That way if I needed to go to bed early, I can still do my late G-tube feeding and prop myself up. It took about five tries to get the equipment provider to get the proper paperwork to my doctor and back again. When we finally got the bed it was not fully automatic as we had requested. It did have a motor to raise and lower the head and feet but it did not have a motor to raise the entire height of the bed. We could have paid the difference in price out of pocket because Medicare/Medicaid would not pay for the fully automatic version but we didn’t discover that until the guy actually delivered the bed. We just decided to live with it as it was. You could manually crank it up or down so we just adjusted it to the height of my old bed and left it there.
As I had speculated, my home health aide Riah had moved on to different clients so we had to train some new people. But they didn’t last very long and eventually we got Riah back again. She continued to work here for nearly 3 years but had to quit a few months ago because of back problems. She hopes to return to work someday and we will welcome her back. We really became very good friends over the past several years and I miss her a lot.
I could fill up a dozen more blog posts about the process of recovery after this incident. It took a long time for me to get back to something similar to my previous normal. Among the things that concerned me was my ability to go out with friends like Rich and Kathy were have friends like the Byram’s or the Brake’s stay with me while dad went to the doctor or did other things. Eventually I got over my concerns and trained them all how to suction my trach and how to do G-tube feedings. I got to the point where I was pretty much back to normal. I thought perhaps my days of going to evening events were going to come to an end but I did eventually attend 2 great concerts at the Deer Creek Music Center with my sister Carol. We also continued to go to hockey games at the Fairgrounds Coliseum but normally try to do afternoon games so it’s easier on me. I continue to go to the movies regularly with my friends Rich and Kathy and we recently saw the final Star Wars film completing a tradition that had lasted 42 years. We have seen every Star Wars movie together (sometimes multiple times) except Rogue One which was playing while I was in the hospital.
The story of my dad’s failing health in 2018 and his death in February 2019 could fill many many more blogs. I’m not sure if I’m up to reliving all of those events. In May 2019 my friend Barbara Alkema and her son Josh moved in with me. That kept me out of a nursing home. My health has deteriorated in the past few months and that has been a big adjustment.
So life continues to send big challenges my way and I do my best to deal with them as they come. I did seriously dedicate myself to documenting the assistive technology such as my iOS switch control and ultimate remote that were so valuable to me in the hospital. I have a new appreciation for what it means to not be able to speak.
Overall the decision to have the trach has kept me alive much longer than I could have without it. It was a good decision to get the trach. It’s allowed me an excellent quality of life and I’m grateful that things like the Passy-Muir speaking valve were invented so that I can continue to be a person with a very strong voice.
The End