This is the ninth in a multi-part blog about my 2 week stay at St. Vincent Seton Specialty Hospital. It’s been several months since I added to this series because I’ve been busy doing other things. However it’s time to make a big push and finally finish the story. There are other major events happening in my life right now so I need to put this behind me and move onto the next chapter. Here is an index to all of the entries in this series.
Training Day
We are now down to December 27, 2016 and this was a banner day that we had been waiting on for a couple of weeks. The respiratory therapist from Home Health Depot was coming to visit to show me all of the equipment we had been waiting weeks to get. He needed to train Dad and Carol on how to use it. Also present were 2 nurses from St. Vincent were going to be visiting me from time to time once I got home. I’m not really sure why they needed to be there since theoretically they should have known how to operate all of this anyway.  12/27/2016 7:30 AM
12/27/2016 7:30 AM
The therapist was a really nice guy named Josh who not only delivered the equipment and trained us, he continued to be our representative for many months. In the first week home he made several visits which eventually tapered off to a monthly visit where he would download data from the ventilator, perform preventive maintenance, and bring us additional supplies.
Josh later went on to do respiratory work in a hospital and was replaced by another guy. We continued to have good people serve this role of the monthly visit to check the machine and to bring us supplies. At one point Home Health Depot sold its business to a company called Lincare which is a terrible company to work with. We ended up switching to a different company called Aerotech and we get good service from them to this day.
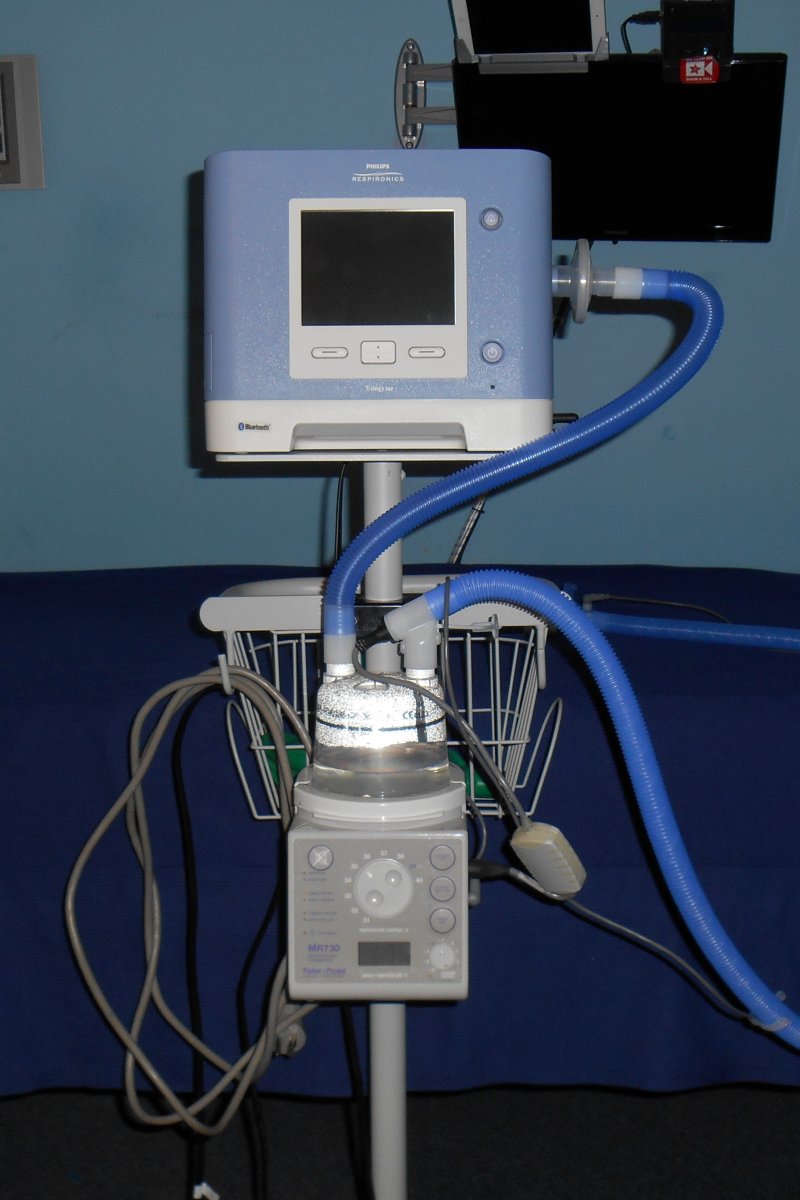
The demonstration and training started off with a ventilator called a Trilogy which from what I’ve learned is one of the most popular small portable ventilators available. I had already done some research about it on the Internet. It’s pretty versatile in that it can be used as a ventilator, CPAP, or BiPAP. It has a backup battery that will last several hours in case of a power failure. It comes a rollaround stand. Just below the ventilator is a humidifier device. It is a small heater that heats up a clear plastic chamber with a metal plate in the bottom of it. You fill the chamber with distilled water and a hose coming out of the ventilator blows through the chamber picking up heat and humidity before going through a hose that connects to your trach.
The ventilator that I had been using in the hospital had 2 hoses coming front it. One was to push the air in and the other let me exhale. They connected to a small Y connector right before they connected to the trach. This ventilator only had one hose. To allow you to exhale, it had a small connector that they call a “whisper swivel”. It is a swivel connector so that the hose doesn’t get twisted but it also has a small gap in it that allows air to escape. If you didn’t have some way to vent your exhaled carbon dioxide you would just keep re-breathing that same gas and would get carbon dioxide poisoning. It’s similar to the tiny hole in my CPAP mask which allows me to exhale. I later learned why it’s called “whisper”. A few months ago we tried out a different type and it made a lot of noise. We stuck with the quiet version.
Jumping ahead in the story a bit… This relatively minor different between the ventilator that I had been using and the one I was going to continue to be using was a bit disturbing the first night. Exhaling felt significantly different. I really wish they had brought the equipment in sooner so that I could get accustomed to it before I left the hospital. As it turned out, the difference wasn’t really that much once I got accustomed to it. But it was a little bit scary the first night when I noticed how it felt different. I wasn’t immediately sure how I would adjust.
The next piece of equipment was a suction machine. This was one of the things that had concerned me the most. Not only was it going to be handy when I needed to spit in the Yankauer, it was also going to be necessary to suction the trach with a catheter. I was concerned about how portable this machine might be. As it turns out it was going to be fine. It fits nicely in a padded cloth case are little larger than a sixpack cooler. It has battery power as well as plug-in. Although it was a little bit larger than I wished it was, I was sure it would work and keep me mobile to go places like visiting family or going to the movies. I have seen other models that were smaller and more portable than this one but I’ve not taken the time to pursue them. This one is working out okay nearly 2 years later.
I was also going to get a small air compressor pump that would provide enough air for a nebulizer treatment. I have been getting these treatments every six hours around the clock. I knew I wasn’t going to do the treatments that often but I wasn’t sure how much I was going to need them. As it turns out I really only need them on as needed basis. I’ve probably only done 8 or 10 of them in the past 20 months.
The one missing piece of equipment was a high flow air compressor that would provide humidity to the trach when I wasn’t on the ventilator. This compressor would use the same humidifier as the ventilator. As I mentioned before, all of the time that I was in bed they insisted I stay on humidified oxygen that would blow into a cup that fits over my trach and talking valve. When I was sitting up in the wheelchair in the hospital I would get off of the humidifier and some days that was okay. However other days I could feel myself drying out thus creating some congestion. In some respects being connected to a humidity source was a kind of dual edged sword. If I became dependent upon it, it would not only restrict my movement away from home but it would also tie me down to one location in my house. On the other hand if it was something I really needed, it was the one thing that wasn’t being addressed despite all of my questions. The respiratory guy from Home Health Depot assured me that he could get me the compressor. All they needed was orders from the doctor that was going to be easy to get.
I’m going to jump ahead and tell the rest of the compressor story out of sequence. While all of the other equipment was reasonably sized and portable, this compressor is a monster that weighed a ton. It was about 2 feet long, a foot tall by about 8 inches deep. It was also very loud compared to the other equipment. For the first couple of weeks, my daily routine was I would get off of the ventilator very early in the morning when Dad would get up about 7 AM. I would then go on the compressor/humidifier until I would get up and dressed and about 10 AM. On rare occasions I may have put it on when I went to bed at about 9 PM and use it until 11 PM when I got on the vent. But eventually I found that it wasn’t necessary at all. It turned out that getting rid of the device was as hard as getting it in the first place. We had a choice of either getting the doctor to rescind his orders or to sign a document saying we were no longer using it against medical advice. Because it was going take a special trip to the doctor just to get those orders changed, at one point I finally just told them to take it and we would sign the AMA form. We made this move when we transitioned from Lincare to Areotech.
I did try one other humidity device. There is a small fitting that you can put on your trach called an HME or Heat and Moisture Exchange device. It sometimes is referred to as an artificial nose because your nose warms and humidifies the air you breathe in. I previously discussed this in an earlier installment. We did end up trying them out and I used them occasionally but not very often and not recently. I still have a huge box of them.
Overall the training went very well and I was satisfied that I was going to get the equipment I needed. Here was my Facebook post from that afternoon which expresses my great relief that we were getting closer to sending me home.  12/27/2016 4:03 PM
12/27/2016 4:03 PM
I stayed in bed that day and got caught up on some other things. Among them I finished editing and posting a blog entry that was top 10 stories of my life for 2016. Here’s a link to that entry.
The other fun thing that happened that day was that I reconnected with Brady Hansen. He was the medical student who had helped care for me when I was in the ICU. I forget the details of how he tracked me down. I believe I had left notes in the ICU for the staff with links to my blog and/or Facebook page. Anyway I got email from him and he had begun reading my blogs about the days in the ICU. He said it was great insights for someone who was about to be a doctor. I encouraged him to share with anyone he wanted. We connected on Facebook and I’ve exchanged a message or two with him from time to time since then. At one point he shared that he was very pleased that he had gotten a residency at a military hospital in California. He had previously been in the military and although it meant moving his family, they were still very excited about it.
The other thing I did that evening was I did some research about the speaking valve that I use. It’s called a Passy-Muir device named after the 2 people who invented it. David Muir was not a designer or engineer or medical professional. He was just a guy with muscular dystrophy who ended up on a ventilator like me and was frustrated that he could not talk. Here is a link to a Facebook post that I made that day about him. It contains a link to a biography page about him. I’m sorry to report he passed away years ago but thanks to his ingenuity I and people like me have a voice. I am greatly indebted to him.  12/27/2016 5:59 PM Click here to read a biography of David Muir. http://www.passy-muir.com/david
12/27/2016 5:59 PM Click here to read a biography of David Muir. http://www.passy-muir.com/david
Being Tested
The final item that we needed to check off before I would be allowed to go home was that Dad had to spend the night with me to prove that he was capable of taking care of me. They brought in a folding bed with wire springs and a rather thin foam mattress completely encased in slick black plastic. They covered it with a sheet that didn’t really fit very well. When you try to sit on it, the sheets would slide around on the slick plastic. The plastic covered mattress on the metal springs made a horrible squeaky noises every time you moved. Later the next day we suggested they ship it to Guantánamo Bay however even Dick Cheney might think it was too harsh of a torture for use on terrorists.
Dad and I were both pretty miffed that he even had to do this. Dad came up with the idea that he was going to make the most of it. If patients in the hospital were entitled to three meals a day and I wasn’t taking advantage of that because of my G-tube, he tried to talk them into bringing him a breakfast tray in the morning as if he were a patient. I tried to tell him he wasn’t going to get very far with that request but he made it anyway. As I expected they were not too keen on the idea and instead told him what hours the cafeteria opened in the morning.
The respiratory therapists from the hospital were in and out that afternoon and evening. They couldn’t help themselves but to play around with the controls and menus on the ventilator even though they’ve never seen one like that before.
In the hospital I had a nurse call button but I’ve spoken about extensively in previous blogs. But during the night, if Dad was going to take care of me, I didn’t want to call the nurse. I needed to call Dad. So we had to bring my call buttons from home. It’s a little Arduino based gadget connected to an X-Bee radio system. It sends a wireless signal from a box in my bedroom to a box in Dad’s bedroom. His box has a loud buzzer on it. So even though we were in the same room, because I can’t talk with the vent on, we needed both boxes so that I could buzz him.
I was concerned that because the buzzer is very loud that it would disturb the other patients or cause the nurses to come running. I wanted to close the door on my room but they said it was against policy to have patients room door closed. We had to leave it open a crack.
Dad had no trouble getting me on the ventilator so we settled down for the night. Every time Dad made the slightest movement his terrible bed made all sorts of squeaky noises. Dad is always a restless sleeper. He tells me that at home he wakes up in the middle of the night with the sheets or covers balled up. With the sheets sliding around on the slippery plastic, it was a wonder he was going to have any sheets at all.
When I’m in bed, they insisted I be connected to an oximetry and heart rate detector. If my oxygen level or heart rate drops below certain levels it rings an alarm. Whatever the default setting is for the heart rate, my sleeping heart rate often goes below that. We’ve been adjusting the level so that it doesn’t trigger so easily. But every time I take the device off and put it back on when I get up in the wheelchair, it resets the defaults. So in the middle of the night, my heart rate went low and the alarm beeped. Dad thought it was me pressing the call button. So he got up trying to ask what I wanted. I had to use my message board with him pointing at various things to try to figure out why I called him. I didn’t have an item on the board saying “I didn’t call you”.
We eventually resorted to taking me off of the ventilator temporarily and putting my speaking valve back in. Then I was able to explain to him what had happened. I don’t recall if we got the nurse or the respiratory therapist to reset the trigger level on the heart rate monitor or not. In the process of taking the off of the ventilator, the ventilator alarm started ringing and we had difficulty figuring out how to reset it. That drew the attention of the respiratory therapist.
It was a wonderful woman about 50 something years old who was my favorite of all the respiratory therapists. I’m embarrassed to say that I don’t for certain remember her name especially because I had grown so fond of her. I guess I didn’t put her name in my notes because I thought that I would never forget her. As I said she was my favorite of the entire two weeks and as you will see played a vital role in getting me out of the place. I’m going to call her Shirley because I know that wasn’t her name and I don’t want her to get in any trouble over the rest of this story.
I don’t recall the exact sequence of events that followed. Shirley was in and out a couple of times. We had explained to her how we got the alarms mixed up. She helped us get everything reset on the ventilator the way it should be.
Somewhere along the way of this entire process of getting me off and on the vent, Dad made a mistake. He made a mistake that we had discussed extensively over a period of days before we ever got to this overnight test. It was the only mistake that you could make with the ventilator that was potentially dangerous so we had discussed it thoroughly. But in the middle of the night when we are both half-asleep or had been sleepless all night as he had been, it’s easy to make mistakes.
The trach has a balloon-like device called a cuff that you have to inflate with air using a small syringe. It cuts off your upper airway above the point of the trach so that when the ventilator blows air into the trach, it doesn’t blowback out through your mouth and nose. The danger is, if you put the talking valve back on the trach without first deflating the balloon, you can’t breathe. In this case Dad was getting ready to put me back on the vent and he inflated the balloon before removing the valve which has the same bad effect. If left there too long it could kill me. As I said, we had discussed the situation thoroughly. We knew we couldn’t guarantee that we would never make that mistake. But we both convinced ourselves that if it happened, he would see that I was in distress and immediately remove the valve allowing me to breathe.
We really didn’t think we would end up making this mistake on the first night. But when it happened, our contingency plan where he would notice my distress and do something about it would have worked perfectly. In fact he was just about to reach to remove the valve so that I could breathe. But there was a problem… Shirley was there. She witnessed it all. And she quickly grabbed the valve before Dad could.
It was as much my fault as it was Dad’s. Shirley was on her way out the door and I thought something else I wanted to say to her. I don’t remember what it was. So I had not noticed that dad was inflating the balloon until it was too late and once it was inflated I could not talk to stop him. If we had been alone, I would not have been distracted and would have reminded him to remove the valve before inflating the balloon.
We were there that night to prove that Dad could handle taking care of me by himself. But when the alarms went off on the vent we had difficulty resetting them. And in the process of trying to get me off of the vent, we made a very serious (potentially fatal) mistake. I knew I was okay the entire time. But what scared the crap out of me was that we had failed the test. I was worried they would not let me go home.
Somehow I managed to get to sleep despite my worries. My estimate is that night I may have gotten five hours sleep. Dad thinks he was lucky if he got three. It was sometime around 5 or 6 AM that I told him to get me off the vent. I knew he had had a terrible night and suggested that he go down to the family lounge down the hall and tried to get some rest in a recliner chair or sofa there. He said that the furniture in that room was no good and he wouldn’t be able to get any rest. We would just have to tough it out the rest of the day.
Then we discussed what we needed to do about Shirley. I told Dad that we needed to explain to her that even though we made some mistakes, we had planned for these mistakes and that we would have been okay without her help. He agreed that we needed to say something to her. Her shift change was at 6 AM so Dad stuck his head out the door and kept his eyes open for her. He flagged her down and we invited her in to talk.
I said approximately the following… “We need to talk about what happened last night. The whole purpose of Dad being here was to prove that he could take care of me on our own. But we had some problems last night that you helped us to resolve. I want to describe to you from our perspective what we think happened last night. When the alarms went off on the ventilator, we had a little difficulty figuring out how to turn them off. The one on the vent is easy. But the one on the humidifier heater is different. Even if you fix the problem, it still keeps beeping until you hit the reset. We’ve got all of the paperwork and instructions here and we would’ve figured out how to reset it eventually. So while we appreciate you helping us out, we are confident we could have handled that part on our own.”
Then I continued with the bigger issue… I said “The other thing that happened last night was that Dad inflated my balloon without removing the valve first. We had talked about this possibility extensively prior to this. We had both convinced ourselves that if we made such a mistake that we would recognize it quickly and we knew exactly what to do to fix it. It just so happened that you were here and fixed it first.” I also explained how I had gotten distracted and did not warn him what was going wrong. I explained if we had been on our own, I would have been more focused and it would have never happened in the first place.
I concluded by saying “From our perspective, that is what happened. We could’ve gotten through all of that on our own. From a different perspective we recognize that it seemed like we didn’t know how to operate the machine and that at one point Kenny nearly killed Chris.” I kind of snickered at that point and she responded by letting out a big laugh.
I went on to say that I realized she was a professional with a responsibility to do what she thought was right. I was not going to ask her to keep this information quiet. “You’ve got to do what you feel is right under these circumstances. This was a test to see if we could handle this on our own. From our perspective we are capable of doing that despite what you saw last night. I just wanted to share with you our perspective on the events and we trust you will do what you think is in our best interest.”
She was totally cool about the whole thing. The first thing she said was that she and every respiratory therapist she had ever known had made that exact same mistake but had only done it once. She said when that happens and you realize it and you fix it, it scares you so bad you know you will never make it again. So you guys have already had your scare. She went on to say she understood what we were saying and that she had every confidence that we would be okay on our own.
If I could have, I would have jumped up out of bed and kissed her full on the lips. 🙂
Hell, I already had kind of a crush on the woman before all of this. That night she saved my life… not by pulling the valve so I could breathe. She saved it by believing in me and Dad and letting us move forward with leaving the hospital and getting on with the rest of our lives. I can’t begin to describe how much she meant to me. She was so genuine in her explanation that I’m not really sure I needed to make the speech I made. Whether or not my words convinced her is irrelevant. In the end, she said nothing and we were able to go home the next day.
Over the past 20 months since then I think we may have done it twice more. In both instances it took less than 5 seconds to realize mistake and fix it. We were right in speculating that we would make the mistake from time to time and we were right that if it happened we could fix it without putting me in any serious jeopardy.
Having passed the necessary test and survived the night. They agreed that I could go home that day. But getting out of a place like that is never easy. Scofield and Burrows on the TV show “Prison Break” have gotten out of prison easier than I did getting out of the hospital. Details in the next installment.